[ad_1]

By Sabrina Corlette, Rachel Swindle, and Rachel Schwab
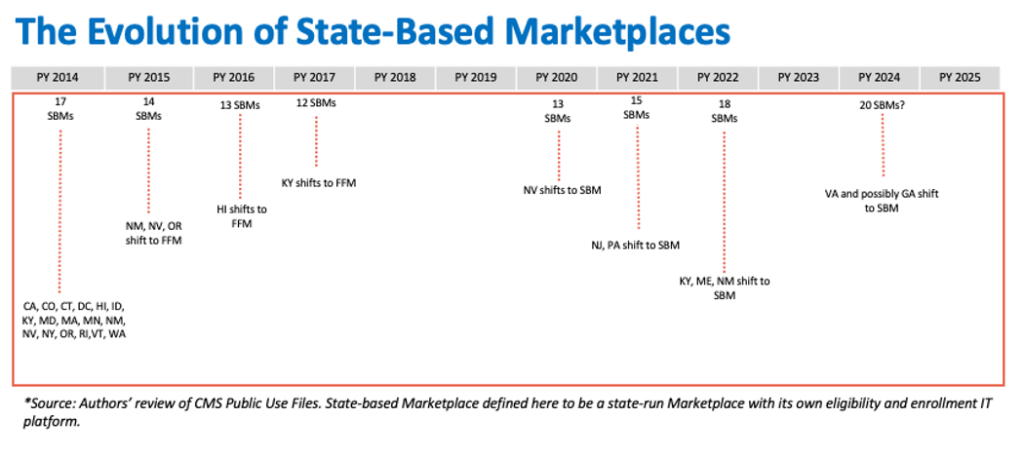
The Reasonably priced Care Act (ACA) established medical health insurance Marketplaces (or “Exchanges”) to facilitate enrollment in complete and inexpensive medical health insurance plans. The ACA envisioned that the Marketplaces could be primarily state-run, with the federal authorities stepping in as a backstop. In apply, due partially to deep anti-ACA sentiment amongst some state policymakers, when the Marketplaces launched in 2013, only 17 states and the District of Columbia had been state-run Marketplaces with their very own IT eligibility and enrollment platforms. The federal authorities needed to run the Marketplaces within the remaining 33 states, and for the reason that inaugural yr, some state-run Marketplaces have used the federal enrollment platform HealthCare.gov. Over the course of the primary decade of the ACA’s Marketplaces, the variety of state-based Marketplaces (SBM) has fluctuated from 17 within the first yr, to a low of 12 in plan yr 2017, to the present 18 in 2023. (See Exhibit). States transitioning to a full SBM lately sought control partially as a result of the Trump administration’s efforts to roll again the ACA led to instability of their insurance coverage markets and an increase in the numbers of uninsured. The power to adapt an SBM to state circumstances and priorities has enabled these states to construct on the ACA and increase enrollment.
Extra not too long ago, a number of further states have indicated they might undertake a transition to an SBM, together with Georgia and Texas, the place opposition to the ACA stays a bedrock precept for a lot of lawmakers. With total Market enrollment at an all-time high, and millions more individuals poised to transition from Medicaid to business insurance coverage, the function of the ACA’s Marketplaces as a well being protection security internet has by no means been extra pivotal. But federal guidelines implementing the ACA impose few requirements for launching and sustaining a Market that adequately serves customers and builds on enrollment beneficial properties. Given states’ interest in taking over operation of the Marketplaces, it could be time for the federal authorities to ascertain a stronger federal ground.
The Want For Minimal Requirements Earlier than Working a State-based Market
So far, SBMs have been main the way in which in direction of better insurance coverage protection and an improved shopper expertise. They’re investing heavily in advertising and marketing, outreach, and enrollment help, coordinating with Medicaid agencies to scale back churn, raising the bar on high quality for collaborating insurers, and appearing to improve the patron buying expertise. Many SBMs have carried out revolutionary methods to achieve the remaining uninsured, resembling state-funded subsidies, protection for undocumented residents, and “easy” or automated enrollment.
Within the final two years, the federally facilitated Market (FFM) has been catching up. The FFM has dramatically increased funding for advertising and marketing and enrollment help. Federal officers have additionally carried out new insurance policies to lengthen enrollment home windows, simplify plan selections, increase eligibility for tax credit (by fixing the “household glitch”), and reduce the quantity of paperwork for customers to take away enrollment obstacles. These efforts are paying off, with record-breaking FFM enrollment in 2023.
Any state in search of to transition from HealthCare.gov to SBM standing in the present day thus has a better threat of backsliding on these protection beneficial properties. The ACA specified that state Marketplaces predating regulation’s enactment, resembling Massachusetts’s Market, had been presumed to qualify below the brand new federal requirements for SBMs provided that they continued to cowl roughly the identical portion of the inhabitants projected to be coated nationally below the ACA. The belief was that SBMs must construct on, not detract from, the ACA’s protection targets.
But not all state leaders in search of to launch an SBM share a dedication to common insurance coverage protection. Certainly, 10 states, together with Georgia and Texas, haven’t taken up the choice to increase Medicaid protection to their poorest residents. And though states are usually the primary line of enforcement of the ACA’s market reforms, Texas has declined to play this function, and as an alternative relies on federal enforcement. Furthermore, Georgia has previously sought permission to bypass a number of key Market necessities, together with the centralized enrollment web site. As a substitute, the state proposed to ship customers to non-public insurers and brokers, each of which have monetary incentives to restrict significant plan comparability.
Market Roles and Obligations
Underneath present federal guidelines, SBMs have an extended record of essential duties, however are topic to comparatively minimal federal requirements for a way they carry out these duties.
Governance
States can set up a Market as a governmental company or non-profit entity. Marketplaces run by impartial state companies and non-profit entities will need to have a governing board certain by a proper and public constitution or by-laws, maintain common and open conferences introduced prematurely, and meet sure membership requirements, resembling a ceiling on members with ties to the medical health insurance business. Market boards should even have publicly out there insurance policies governing conflicts of curiosity and monetary curiosity disclosures, ethics rules, and accountability and transparency requirements. Federal guidelines implementing the ACA don’t specify the variety of instances Market boards should meet yearly, how far prematurely conferences have to be introduced, the variety of people on the governing board, if there are time period limits for voting board members, or how board members are chosen or appointed.
Funding
In establishing a Market, states should guarantee it’s financially self-sufficient. States have broad flexibility to decide on the mechanism by which they fund their Market, resembling an evaluation or payment on insurers or a state appropriation of different funds. States can also apply for future federal grants, resembling when Congress allocated further funding below the American Rescue Plan Act (ARPA).
Stakeholder Session
The ACA requires Marketplaces to seek the advice of with stakeholders on a “common and ongoing foundation,” together with Market enrollees, people and entities facilitating Market enrollments, small companies representatives, the state’s Medicaid company, “advocates for enrolling onerous to achieve populations,” federally acknowledged Tribes, public well being consultants, suppliers, massive employers, insurers, and brokers/brokers. Federal guidelines don’t specify the frequency or type for stakeholder session, which elements of the Market operations are topic to stakeholder enter, or a course of to make sure stakeholder suggestions is included into Market insurance policies and practices.
Extra Than a Web site
The Marketplaces should carry out a number of capabilities designed to make sure that customers are capable of perceive their choices, decide their eligibility for premium tax credit, and enroll in a well being plan that meets minimal requirements. These capabilities embrace:
Plan Administration. States that function their very own Marketplaces are accountable for certifying that well being plans are “certified well being plans” (QHPs), merchandise eligible to be bought on the Market. This implies the plans should meet federal and state profit necessities, premium ranking guidelines, prescribed “actuarial worth” or plan generosity ranges, prohibitions in opposition to discriminatory profit design or pre-existing situation limitations, and community adequacy, amongst different requirements. Whereas some necessities apply to plans in each Market, others, resembling particular community adequacy requirements, differ relying on whether or not the Market is state- or federally run. Some Marketplaces that function independently of their state division of insurance coverage (DOI) nonetheless depend on their DOI for sure plan administration duties.
On-line Eligibility and Enrollment Platform. Marketplaces should keep a web site for customers to buy and enroll in protection in a manner that’s accessible for these with disabilities and/or restricted English language proficiency. Web sites should present, for instance, standardized details about QHPs to facilitate plan comparability, together with premium and cost-sharing particulars, a shopper price calculator, a abstract of advantages and protection for every product out there, high quality rankings, and supplier directories. Market web sites additionally function an entry level for different insurance coverage affordability applications, resembling Medicaid, both by working a full eligibility willpower or directing customers to the suitable state company. The character of medical health insurance enrollment additionally requires Marketplaces to gather delicate private data, and accordingly Marketplaces should meet federal privateness requirements or face financial penalties.
Lots of the first Market web sites had been a disaster, leading several to pivot to the FFM in their first year. Since then, both federal and state platforms have improved considerably and successfully enrolled millions of consumers. However, the ongoing maintenance and operation of these websites requires a considerable investment. Federal policy changes, such as the recent premium subsidy enhancements in ARPA and the Biden administration’s “family glitch” repair, can even require speedy and costly updates to on-line eligibility methods. In each of these cases, some SBMs weren’t capable of make the required modifications to their web sites in a well timed vogue.
Market Name Facilities. SBMs are required to function a toll-free name middle to discipline questions and requests from customers in regards to the eligibility and enrollment course of. Apart from the requirement to have a toll-free name middle, federal guidelines don’t impose exacting requirements on Marketplaces, resembling staffing ranges or most name wait instances. Some Market name facilities have skilled system outages and significant wait times throughout their annual enrollment intervals. Up to date, clear federal requirements and ongoing oversight of customer support high quality might assist keep away from comparable points sooner or later.
Outreach and Enrollment Help. Federal laws require SBMs to “conduct outreach and training actions . . . to teach customers in regards to the [Marketplace] and insurance coverage affordability applications to encourage participation.” Apart from being accessible for individuals with restricted English proficiency and folks with disabilities, SBMs have vital flexibility in how and to what extent they conduct this outreach.
SBMs are required to run and fund their very own Navigator applications, though federal guidelines depart many of the particulars of these applications to the states. As an illustration, though all Marketplaces should set up sure coaching requirements (resembling coaching on assembly the wants of underserved populations), states can decide the content material and frequency of these trainings.
Federal guidelines additionally don’t set up a minimal funding stage required for both Navigator applications or outreach campaigns. Because of this, there’s a wide range of SBM funding ranges in these proven tactics for rising protection.
Course of for Transitioning to a State-Primarily based Market
The method for transitioning to an SBM usually requires the state to submit two primary elements to the federal authorities: (1) a letter declaring the intent to transition, and (2) an “Exchange Blueprint” to show the state’s potential to function a Market. Federal regulators have made some changes to the Blueprint through the years, most notably permitting states to easily attest that they meet most of the federal necessities to function a Market as an alternative of submitting documentation offering proof of compliance. And, regardless of stakeholder concern, starting in 2024 Blueprint approval is no longer required at the least 14 months previous to the beginning of the brand new SBM’s preliminary open interval, permitting for a shorter timeframe between federal approval and an SBM turning into operational to serve customers.
Setting a Bar: Potential Minimal Requirements
With out further minimal requirements for the design and operation of an SBM, there’s a threat that the patron expertise with the Market will worsen, making enrollment more difficult and in the end lowering protection charges. Whereas the ACA clearly envisions a excessive diploma of state autonomy over the operation of the Marketplaces, just a few further requirements for SBMs might embrace, for instance:
- A deliberative SBM transition course of. Hiring employees with the required abilities and experience, procuring the required IT and different service suppliers, testing methods, constructing model consciousness, and interesting with assisters, carriers, and different stakeholders all take time. Given the stakes for customers, it’s not a course of that ought to be rushed. It may be useful for states to spend a minimal of 1 yr as an SBM on the federal platform (SBM-FP) earlier than absolutely transitioning to an SBM. This would offer a while for CMS to evaluate the state’s method to governance, shopper outreach and help, and stakeholder engagement, earlier than handing over full management.
- Transparency and neighborhood engagement. States ought to be soliciting and incorporating public touch upon their proposed Blueprint, and publicly posting their Blueprint purposes. Better transparency surrounding SBMs’ income supply(s) and spending, resembling extra distinguished public posting of audits, in addition to knowledge on key metrics resembling plan alternatives, effectuated enrollments, name middle wait instances, and spending on Navigators and shopper help can also be essential.
- An funding in shopper outreach and help. Given the confirmed effectiveness of shopper outreach and help, it will likely be vital for SBMs to satisfy minimal efficiency requirements for shopper outreach, name middle assist, and Navigator applications.
- Requirements for Market well being plans. Enrollees in all Marketplaces need to have plans that meet minimal standards for certification. Though CMS has so far shunned extending some requirements, resembling community adequacy, to insurers in SBM states, a federal ground might be useful to keep away from a large divergence in shopper protections throughout states. At a minimal, if a state isn’t implementing the ACA market reforms, it shouldn’t be working an SBM.
Trying Forward
So far, states have chosen to function their very own Market based mostly on a dedication to inexpensive, complete medical health insurance for all their residents, with the SBM serving as a essential software for reaching that objective. However in some states that will search SBM standing sooner or later, significantly those who have demonstrated antagonism in direction of the ACA’s protection expansions and shopper protections, additional federal guardrails might assist scale back the chance of a decline in customers’ expertise and, within the worst-case state of affairs, a reversal of the latest beneficial properties in insurance coverage protection.
The authors thank Justin Giovannelli, Jason Levitis, Sarah Lueck, Claire Heyison and Tara Straw for his or her considerate overview and modifying of this submit.
[ad_2]



